Where did monkeypox come from?
A close up look at the original paper documenting its discovery.
According to the WHO, monkeypox is a zoonotic virus belonging to the ‘orthopoxvirus’ family. It is said to be similar to smallpox, but “less contagious” and causing “less severe illness”.
The symptoms are virtually identical to those of smallpox and other pox viruses (for a long time, smallpox, chickenpox and shingles were thought to be the same disease).
Other than mortality rate and infectiousness, we are told the main difference between monkeypox and these other viruses is that monkeypox causes lymphadenopathy (swollen lymph nodes).
However, lymphadenopathy can also manifest in cases of chickenpox (see here and here).
The CDC emphatically states that “the main difference between symptoms of smallpox and monkeypox is that monkeypox causes lymph nodes to swell (lymphadenopathy) while smallpox does not.” The monkeypox fact sheet published by the Virginia department of health states that swollen lymph nodes are “not usually seen in smallpox”.
Historically, little attention has been paid to lymph nodes when examining smallpox cases, but there are some examples: “when death occurs in the second week the mesenteric nodes, and occasionally the cervical, the aortic, and the inguinal, may show some swelling. In cases fatal during the third week changes in the lymph nodes are rare; in one the cervical nodes were somewhat enlarged.”
Given the above, it’s surprising that anybody would confidently assert that lymphadenopathy was not commonly found in smallpox cases. The CDC also state that lymphadenopathy is a common side effect of smallpox vaccines. And what’s more, this apparently distinctive feature of monkeypox doesn’t manifest in 10% of cases.
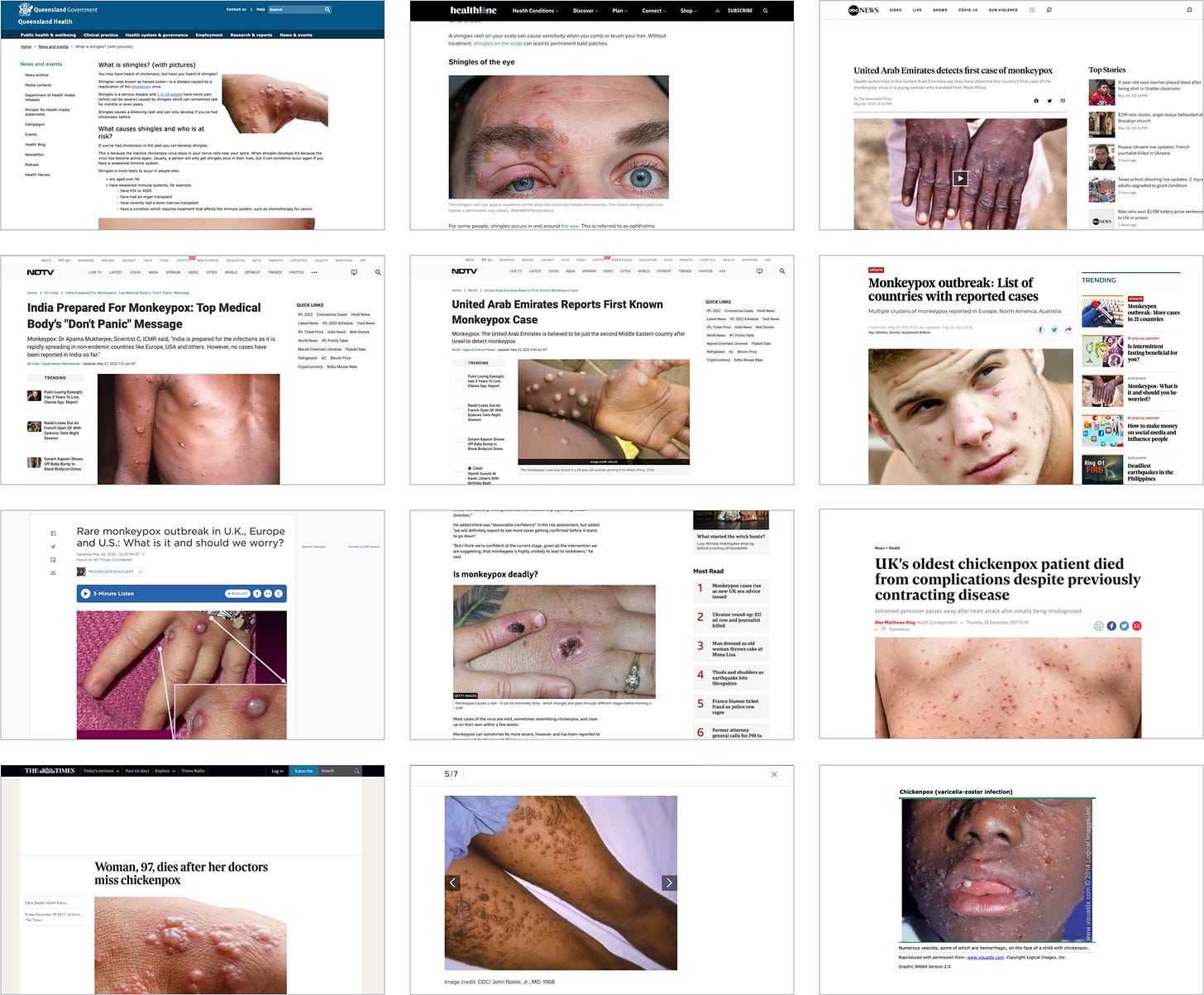
Interestingly, the aforementioned health authorities make no mention of the monkeypox rash being any worse than other Orthopoxvirus rashes, and whilst some seem to be under the impression that this rash is somewhat distinctive, we also find that it varies in its appearance quite significantly, and that in some cases, it isn’t all too dissimilar from cases of shingles.
On the surface, it is unclear what defines monkeypox as a different disease within its class.
Scientists will tell you they most certainly are clear of the difference, because they’ve discovered the virus, characterised it and, most importantly, demonstrated that it causes this specific disease.
How was this done?
Discovering the monkeypox virus
Monkeypox was discovered by a research team in 1958, in Copenhagen.
The lab was receiving a continuous supply of monkeys for the purpose of polio vaccine production and research. Upon reception, the monkeys were given penicillin and streptomycin, it would appear, to try and prevent pneumococci infection.
Rashes are a known side effect of penicillin, and again, these appear to vary greatly in their appearance.
At the time, all polio vaccines, with the exception of one, contained penicillin. And on occasion, this was shown to cause a reaction. For instance, this paper, published in 1959, details the case of an individual who had a reaction that included “generalised giant urticaria” – a type of rash, described here as consisting of “blancheable, erythematous, oedematous papules or ‘weals’” that are “usually intensely itchy”. This later progressed to a rash that was said to resemble German measles.
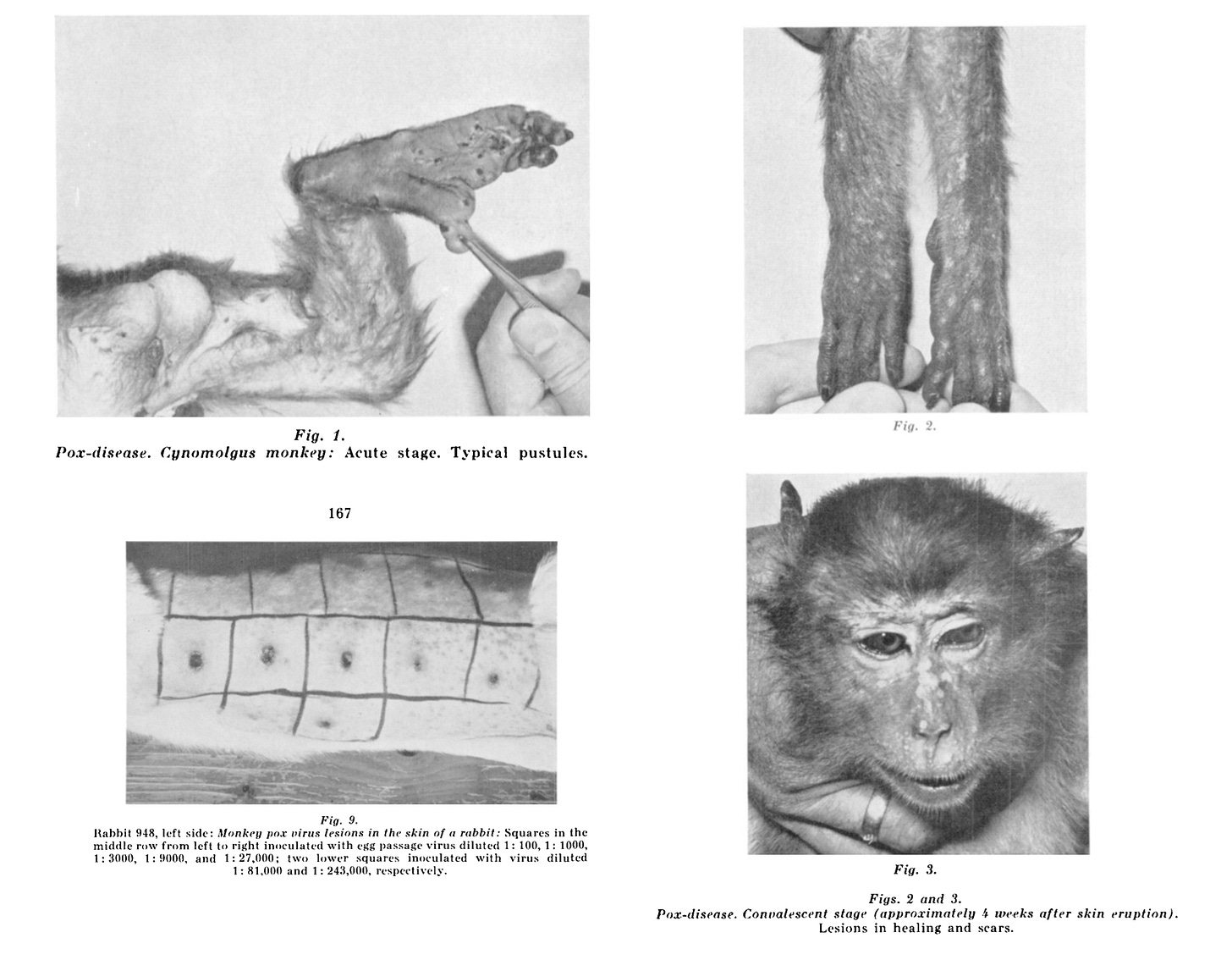
Going back to our monkeypox paper, the researchers state that: “both outbreaks occurred late after arrival of the monkeys, i.e. after 51 and 62 days, respectively, and only 20 to 30 per cent of the animals developed clinical signs of disease.”
They further state that “the clinical manifestations were characterized by skin eruptions of a maculo-papular rash and of various pustules. The general health of the animals was not seriously affected and fatal cases were not observed…. Judging from the scratched appearance of several of the lesions, particularly on the back of the animals, it seemed likely that the eruption was associated with some itching.”
After the outbreak, the virus was isolated: “pustular scrapings were emulsified in tryptose-broth, clarified by low speed centrifugation, and the supernatant was inoculated into tissue cultures of monkey kidney, human amnion, and HeLa cells.”
It is difficult to see how the above process would result in a complete separation of the virus from all other contaminants, but let’s put that aside.
Testing the contagion hypothesis
Unless you are able to demonstrate that pathogen A causes disease B, you cannot assert that the particle you have found in diseased subjects is, indeed, the cause of a given disease, and not a byproduct.
A perfect case in point is that of the SMON epidemic. A unique virus particle was discovered (see here, here and here), but it was eventually concluded that the disease was caused by the drug, clioquinol.
Correlation is not causation. A good analogy is that of flies and roadkill. One often finds them together, but the flies did not kill the animal.
According to the CDC, transmission of monkeypox is said to occur through skin contact and aerosol. So, in order to demonstrate transmission, you would need to attempt to replicate what happens in the ‘real-world’ – like the experiments carried out during the Spanish flu epidemic, where multiple infection routes were attempted, including asking volunteers to cough in each other’s faces. Interestingly, none got sick.
In the case of monkeypox, the researchers tried to transmit the virus to other lab animals. The experiments involved completely unnatural forms of transmission – mainly, injections. For example: “depilated rabbits were inoculated with 0.1 ml amounts of serial dilutions of monkey virus. The severe hemorrhagic reactions which developed were very different from those caused by vaccinia virus”.
Adult mice were also used, but for some reason intracerebral inoculations were necessary. Last but not least, the experiment was carried out on 2 monkeys. These received an intradermal injection. The researchers report that “none of these animals developed any signs of illness”, but that “one cynomolgus monkey … developed a local pustule surrounded by oedema 7 days after inoculation. Attempts to re-isolate virus from the lesions were unsuccessful because of heavy contamination with molds and bacteria.”
The researchers concluded their study by saying that they are ‘puzzled’ by the lengthy period of time that elapsed between the monkeys arriving and the outbreak – and that the lesion in the one reactive monkey developed only 7 days after inoculation.
All of this is certainly very puzzling. For a start, why were injections needed? It may come as a surprise to some to find out that this is how virtually all such experiments are carried out (see for instance the thread I wrote on smallpox, chickenpox and shingles – where, among other things, we learn about how virologist Thomas Rivers used ground up rabbit testicles mixed with sand, which he then injected into the testicles of other rabbits to try and demonstrate contagion).
Why did this disease only manifest after the monkeys had spent time in the lab? Are we supposed to completely disregard the fact we don’t know all the details of what happened to the monkeys whilst they were being held in captivity? Has this disease ever been seen in monkeys in the wild? If so, how do we know it was caused by a virus, and not by exposure to an environmental toxin?
On this point, a primatologist told me: “I've worked with thousands of monkeys and apes; never seen or heard of a case. If you put them in a cage and stress the hell out of them they get sick, pull hair out, even die. That's without pumping them full of inoculants.”
What could have caused the ‘severe hemorrhagic reactions’ in the rabbits? What else was in the substance they were inoculated with?
Last but not least, the distinct lack of controls is somewhat baffling. If we were to repeat these exact experiments using non-contaminated materials, what would we expect to see?
If you were to inject a solution – any solution – into the brain of a mouse, what do you think would happen?

Great article. There's a very large mammal in the room and it ain't no monkey.
Milton Rosenau's experiment along with those artic or sea explorers who went down with 'flu' months out of contact from any reasonable vectors occupy my thoughts a lot. Like the absurdity of injecting sand into testicles or tinctures into brains and blaming invisible things for the harm caused. A child can see through the pharmakeia's trick, while learned adults are baffled by the complexity they themselves create to obfuscate the obvious.